As we move further into 2026, the conversation around mental health and addiction treatment is undergoing a profound transformation. Psychedelics, once relegated to the fringes, are now at the forefront of therapeutic innovation. Their potential to unlock deep healing and facilitate lasting change is becoming increasingly undeniable, offering new hope for individuals struggling with a range of conditions.
Among these powerful substances, ibogaine stands out for its unique properties, particularly in addressing severe addiction. This article delves into the evolving role of psychedelic healing, with a specific focus on ibogaine’s advancements and accessibility in Canada by 2026.
Beyond the Horizon: Emerging Trends in Psychedelic Wellness in 2026
The Shifting Landscape of Mental Health Support
In 2026, the paradigm for mental health support is decisively shifting from symptom management to root-cause resolution. Traditional therapies, while valuable, are increasingly being complemented by innovative approaches that leverage the neuroplasticity-enhancing effects of psychedelic compounds. This evolution is driven by growing clinical evidence and a greater societal acceptance of non-traditional healing modalities. We are seeing a rise in integrated care models, where psychedelic-assisted therapy is combined with psychotherapy and lifestyle interventions to create a holistic recovery plan. This comprehensive approach aims not only to alleviate distress but also to foster profound personal growth and well-being. The focus is on empowering individuals with tools for sustained mental resilience, moving beyond a model of mere “fixing” to one of genuine thriving. The accessibility of these therapies is also expanding, with more insurers beginning to recognize their efficacy, albeit slowly.
The demand for personalized wellness solutions is also fueling the growth of psychedelic wellness. Beyond clinical settings, microdosing protocols and guided psychedelic experiences for personal development are gaining traction, though often within unregulated spaces. Decision-making criteria for individuals exploring these options include clear intentions, careful preparation, and integration support. Pitfalls to avoid involve self-medication without proper guidance, underestimating the intensity of the experience, and neglecting post-session integration, which is crucial for lasting benefits. For example, an individual struggling with persistent anxiety might explore microdosing psilocybin, focusing on cultivating presence and reducing rumination. The actionable step here is to seek out facilitators or therapists trained in psychedelic-assisted approaches, ensuring safety and maximizing therapeutic outcomes.
The broader trend also encompasses the destigmatization of psychedelics, moving them from illicit substances to potential therapeutic agents. This shift is supported by research into their efficacy for conditions like PTSD, depression, and anxiety, offering a glimmer of hope for those who haven’t responded to conventional treatments. Psychedelics for mental health are no longer a fringe concept but a burgeoning field of scientific inquiry and therapeutic application, promising a more compassionate and effective future for mental healthcare.
Canada’s Evolving Approach to Psychedelic Therapies
Canada has emerged as a leader in exploring and integrating psychedelic therapies into its healthcare framework. While not yet fully mainstream, significant strides have been made in allowing regulated access for specific conditions. Health Canada’s Special Access Program (SAP) has been instrumental, enabling physicians to apply for access to substances like psilocybin and MDMA for patients with life-threatening illnesses or those who have exhausted all other treatment options. This program represents a crucial bridge between research and clinical practice, acknowledging the profound potential of these compounds under medical supervision. The emphasis remains on rigorous scientific study and ethical implementation, ensuring patient safety and maximizing therapeutic benefit. This cautious yet progressive approach is setting a precedent for other nations considering similar pathways.
The legal and regulatory landscape continues to adapt, with provinces like Alberta and British Columbia showing particular openness to innovative mental health treatments. While widespread public funding for psychedelic therapies is still nascent, private clinics and research institutions are actively contributing to the evidence base. Decision-making for policymakers and healthcare providers involves balancing patient access with robust safety protocols and ethical considerations. Potential pitfalls include the risk of unregulated or unqualified practitioners offering services, leading to negative experiences or harm. Actionable steps involve advocating for clear regulatory frameworks, investing in training for mental health professionals, and supporting research initiatives that can provide definitive efficacy data.
Examples of progress include the establishment of dedicated research centers focused on psychedelic science and the increasing number of clinical trials exploring their therapeutic applications for conditions ranging from depression to end-of-life distress.
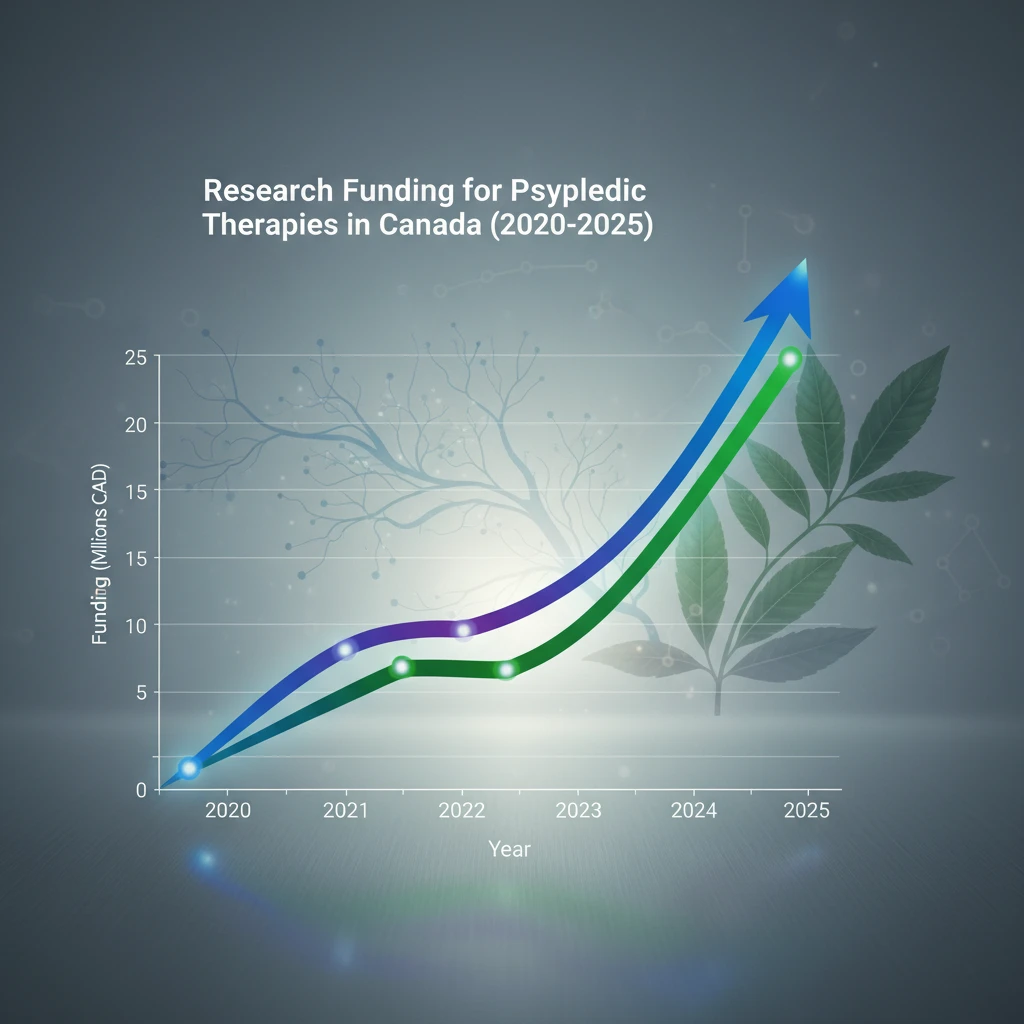
This evolving approach highlights Canada’s commitment to exploring novel avenues for mental health improvement.
Ibogaine: A Deeper Dive into its Therapeutic Potential
Understanding the Science Behind Ibogaine’s Effects
Ibogaine, derived from the root bark of the African Tabernanthe iboga shrub, is a unique psychoactive compound with profound effects on the brain and consciousness. Its therapeutic potential is largely attributed to its complex interaction with multiple neurotransmitter systems. Unlike many psychedelics that primarily target serotonin receptors, ibogaine also interacts with dopamine, NMDA, and opioid receptors, contributing to its multifaceted effects. This broad engagement is thought to underlie its efficacy in treating addiction, particularly opioid dependence, by modulating reward pathways and reducing withdrawal symptoms. The substance is also recognized for its potential to facilitate introspection and personal insight, often described as a “life review” experience, which can be crucial for psychological healing.
Research in 2026 continues to illuminate the intricate neurobiological mechanisms through which ibogaine exerts its effects. Studies are focusing on its role in neurogenesis, the growth of new neurons, and synaptic plasticity, the brain’s ability to form new connections. These processes are critical for overcoming ingrained patterns of behavior and thought associated with addiction and other mental health challenges. Decision-making in research circles involves prioritizing studies that elucidate these mechanisms to guide clinical application safely and effectively. Pitfalls include oversimplifying its action or extrapolating findings from animal models directly to human outcomes without rigorous clinical validation. Actionable steps involve continued investment in advanced neuroimaging techniques and biochemical analyses to map ibogaine’s precise pathways in the brain.
The experience itself is often described as profoundly introspective and can last for many hours. It is characterized by vivid visions, emotional release, and a deep re-evaluation of one’s life and past experiences. This process, while potentially challenging, is believed to be integral to the transformative healing that ibogaine can facilitate. Understanding this intricate interplay of neurochemistry and subjective experience is key to unlocking ibogaine’s full therapeutic promise. For those interested in its potential, exploring resources like understanding ibogaine provides a solid foundation.
Pharmacological Profile and Mechanism of Action
Ibogaine’s pharmacological profile is exceptionally complex, distinguishing it from many other psychoactive substances. Its primary psychoactive metabolite, noribogaine, is responsible for many of its enduring effects and also contributes to its long half-life. While ibogaine itself interacts with a wide array of receptors, including serotonergic, dopaminergic, adrenergic, and cholinergic systems, its influence on the NMDA receptor system and its interaction with opioid receptors are particularly significant for addiction treatment. This multi-target action allows it to disrupt the neurobiological adaptations that underpin substance dependence, including the downregulation of dopamine receptors and the sensitization of reward pathways. The goal is to reset these systems, thereby reducing cravings and the compulsion to use.
The mechanism of action also involves the upregulation of brain-derived neurotrophic factor (BDNF), a protein crucial for neuronal survival, growth, and plasticity. Increased BDNF levels are associated with improved mood, cognitive function, and the ability to form new, healthier neural pathways. Decision-making in therapeutic contexts involves carefully assessing a patient’s cardiac health due to ibogaine’s potential cardiovascular effects, such as QT interval prolongation. Pitfalls include administering ibogaine without thorough medical screening or in environments lacking appropriate medical support, which can lead to serious adverse events. Actionable steps involve standardizing screening protocols, developing advanced monitoring techniques during treatment, and further research into the synergistic effects of ibogaine with other therapeutic agents.
Furthermore, preliminary research suggests that ibogaine may have neuroprotective properties and could potentially counteract some of the neurotoxic effects of chronic substance abuse. This dual action of neurological repair and addiction interruption makes it a compelling candidate for treating complex addiction disorders.
The scientific community continues to explore these intricate mechanisms to optimize its therapeutic application.
The Ibogaine Experience: What to Expect
The ibogaine experience is often described as a profound journey into the self, characterized by intense introspection, vivid visual and auditory hallucinations, and a deep emotional catharsis. It typically begins with a period of physical discomfort, including nausea and potential motor coordination issues, often preceding the onset of visionary states. These visionary states can range from abstract patterns to detailed replays of past memories and life events. Many describe it as a “life review,” offering a unique perspective on personal history, past traumas, and the root causes of their present challenges, particularly addiction. The duration of the active visionary phase can vary significantly, generally lasting between 6 to 24 hours, with residual effects lasting for days.
Decision-making regarding the setting and support during an ibogaine experience is paramount. It is crucial to undergo treatment in a safe, controlled environment with experienced facilitators and medical personnel present. Pitfalls include attempting self-treatment, undergoing treatment in an unregulated setting, or not having adequate post-treatment integration support. The intensity of the experience necessitates careful preparation and a strong intention for healing. Actionable steps involve thorough pre-treatment screening, including psychological assessments and medical evaluations, followed by a commitment to integration therapy post-experience. This integration phase is vital for processing the insights gained and translating them into lasting behavioral changes.
Common subjective reports include a sense of detachment from the physical body, encountering spiritual or archetypal figures, and experiencing a profound sense of interconnectedness. Many individuals report a significant reduction in cravings for their substance of choice following the experience, alongside a renewed sense of purpose and clarity. The aftermath often involves a period of heightened emotional sensitivity and introspection, making integration support essential. For those seeking to understand more, resources on ibogaine treatment offer comprehensive guidance.
Addressing Addiction: Ibogaine’s Impact in 2026
Case Studies: Long-Term Successes in Addiction Recovery
In 2026, a growing body of evidence highlights the long-term efficacy of ibogaine treatment for severe addictions. Numerous case studies illustrate individuals who, after years of struggling with substances like opioids, stimulants, and alcohol, have achieved sustained sobriety following ibogaine therapy. These successes are often characterized by a dramatic reduction or complete cessation of cravings, a significant improvement in overall mental health, and a restoration of quality of life. For example, a hypothetical case study might involve “John,” a 45-year-old individual with a 20-year opioid addiction history. After a single ibogaine-assisted session in a controlled clinic setting, John reported a complete absence of opioid cravings for over two years, enabling him to rebuild his relationships and career. Such examples underscore the potential of ibogaine to offer a profound reset.
Decision-making for individuals considering ibogaine for addiction hinges on the severity and duration of their dependence, as well as their willingness to engage in a rigorous therapeutic process. Pitfalls include expecting a magical cure without commitment to integration and lifestyle changes, or not selecting a reputable clinic with experienced medical and psychological support. Actionable steps involve thorough research into treatment centers, open communication with healthcare providers, and a commitment to follow-up care, including psychotherapy and support groups. The focus extends beyond the acute detoxification phase to long-term recovery and relapse prevention. Understanding various treatment options is crucial, and resources on expert guidance for ibogaine treatment can be invaluable.
Another illustrative, albeit hypothetical, example could be “Sarah,” who struggled with severe alcohol addiction for over a decade. Following an ibogaine-assisted protocol, she experienced a significant reduction in her desire for alcohol and gained profound insights into the underlying emotional issues that contributed to her drinking. Two years post-treatment, Sarah remained sober, actively engaged in her recovery, and reported a level of psychological well-being she hadn’t experienced in years. These narratives, while individual, collectively point towards ibogaine’s unique capacity to disrupt addictive patterns and facilitate lasting change when administered responsibly.
The Neurobiological Basis for Ibogaine’s Anti-Addictive Properties
The anti-addictive properties of ibogaine are increasingly understood through its complex interactions at the neurobiological level. Central to its action is its ability to modulate the mesolimbic dopamine system, which is critically involved in reward, motivation, and addiction. Chronic substance use often leads to dysregulation of this system, characterized by blunted dopamine responses to natural rewards and heightened responses to the drug of choice. Ibogaine, through its interaction with dopamine D2 receptors and its influence on other neurotransmitter systems, appears to help reset these altered reward pathways. This resetting mechanism is believed to reduce drug cravings and the compulsive drive to seek and use the substance, thereby interrupting the addiction cycle.
Further research in 2026 is investigating ibogaine’s role in neuroplasticity and neurogenesis, particularly within areas of the brain affected by addiction, such as the prefrontal cortex and nucleus accumbens. Its ability to promote the expression of factors like BDNF and GDNF (glial cell line-derived neurotrophic factor) is thought to facilitate the repair of neural circuits damaged by substance abuse and to support the formation of new, healthier connections. Decision-making in research aims to pinpoint the precise molecular targets and pathways that mediate these neuroregenerative effects. Pitfalls include attributing all of ibogaine’s effects solely to one mechanism, neglecting the interplay between different neurotransmitter systems and downstream signaling cascades. Actionable steps involve utilizing advanced molecular biology techniques and longitudinal neuroimaging studies to track these changes over time.
Moreover, ibogaine’s interaction with opioid receptors, including its partial agonism at mu-opioid receptors and antagonism at kappa-opioid receptors, contributes to its effectiveness in treating opioid dependence. This complex interaction can help alleviate opioid withdrawal symptoms and disrupt the persistent withdrawal-induced neurochemical adaptations that fuel relapse. The combination of these neurobiological effects – resetting reward pathways, promoting neuroplasticity, and modulating opioid system interactions – provides a compelling scientific rationale for ibogaine’s powerful anti-addictive potential.
Comparison with Conventional Addiction Treatments (Focus on Efficacy Data)
When comparing ibogaine to conventional addiction treatments, it’s crucial to examine efficacy data across different substance use disorders. Conventional methods, such as agonist/antagonist therapies (e.g., methadone, buprenorphine for opioids), behavioral therapies (e.g., CBT, contingency management), and 12-step programs, have demonstrated varying degrees of success, with relapse rates remaining a significant challenge. For instance, while methadone can effectively reduce opioid cravings and withdrawal, it often involves long-term maintenance with its own set of challenges and potential side effects. Behavioral therapies are essential for addressing underlying psychological issues but may require extensive duration and patient engagement to yield significant results.
Ibogaine’s unique appeal lies in its potential for rapid, and in some cases, single-dose intervention for addiction, particularly opioid and stimulant use disorders. Studies, though often from less controlled settings than traditional pharmaceutical trials, have reported high rates of sustained abstinence following ibogaine treatment. For example, some retrospective studies have indicated abstinence rates of 40-70% at 6 months to 1 year post-ibogaine, compared to significantly lower rates for some conventional approaches, especially for severe, long-standing addictions. Decision-making in this comparative analysis involves acknowledging the limitations of available ibogaine research, such as smaller sample sizes and varied treatment protocols. Pitfalls include directly comparing efficacy without accounting for the different patient populations, treatment durations, and intensities. Actionable steps involve rigorous, placebo-controlled clinical trials for ibogaine to establish its efficacy within standardized medical frameworks, allowing for more direct and reliable comparisons.
It’s important to note that ibogaine is not a universal panacea and may not be suitable for everyone. Its potential risks, particularly cardiac issues, necessitate careful medical screening, which is often more intensive than for many conventional treatments. However, for individuals who have failed to achieve sustained sobriety with traditional methods, ibogaine represents a powerful alternative with a compelling neurobiological basis and promising, albeit still developing, efficacy data. Further exploration of expert guidance on ibogaine treatment in Canada is recommended for those considering this path.
Navigating Ibogaine Therapy in Canada Today
Legal Status and Accessibility of Ibogaine Treatment in Canada
In 2026, the legal status of ibogaine in Canada remains complex, operating in a nuanced space between prohibition and regulated access. While ibogaine is not explicitly scheduled under the Controlled Drugs and Substances Act for therapeutic use, its possession and distribution without proper authorization can carry legal risks. However, Health Canada has provided pathways for exceptional access through the Special Access Program (SAP), allowing physicians to request ibogaine for patients with life-threatening conditions or those who have exhausted all other treatment options. This program, while limited, signifies a governmental acknowledgment of ibogaine’s therapeutic potential. Private clinics operating within Canada often navigate these regulations by sourcing ibogaine internationally and administering it under strict protocols, though the regulatory oversight for these private facilities can vary.
Accessibility is further shaped by the significant cost associated with ibogaine treatment, which is generally not covered by public healthcare plans or most private insurance. This financial barrier means that many individuals seeking ibogaine therapy must rely on personal savings, crowdfunding, or specialized loans. Decision-making regarding accessibility involves weighing the potential benefits against the substantial financial investment and the inherent risks associated with a powerful substance. Pitfalls include the emergence of unregulated or underground “ibogaine providers” who may lack the necessary medical expertise and safety protocols, putting individuals at serious risk. Actionable steps involve advocating for clearer regulatory frameworks that define safe and legal access to ibogaine for therapeutic purposes, potentially through expanded clinical trials or specific licensing for qualified practitioners and clinics.
The landscape is dynamic, with ongoing discussions and advocacy efforts aimed at improving access and clarity. Organizations and researchers are working to build a more robust evidence base, which could eventually influence policy changes. For individuals interested in exploring their options, understanding the current legal framework and the available avenues for treatment is the first critical step. Many find it helpful to consult resources that detail how to find ibogaine treatment in Canada, providing guidance on navigating the complexities.
Finding Reputable Ibogaine Clinics in Canada
Identifying reputable ibogaine clinics in Canada requires a diligent and discerning approach, given the substance’s unique therapeutic profile and the varying levels of regulation. A reputable clinic will prioritize patient safety above all else, employing a multidisciplinary team that includes medical doctors, nurses, addiction specialists, and experienced psychedelic therapists. Decision-making criteria should include the clinic’s adherence to strict medical protocols, including comprehensive pre-treatment screening for cardiac health (e.g., ECGs, Holter monitoring) and psychological readiness. Pitfalls to avoid are clinics that downplay the risks of ibogaine, lack qualified medical staff, or operate without proper licensing and oversight. Transparency regarding treatment protocols, dosages, and potential side effects is also a key indicator of a trustworthy establishment.
Actionable steps for finding a reputable clinic include thorough online research, reading independent reviews (while being mindful of potential biases), and seeking recommendations from trusted sources within the psychedelic or addiction recovery communities. Direct communication with the clinic is essential; schedule consultations to discuss their approach, ask detailed questions about their medical support staff, emergency preparedness, and post-treatment integration services. Be wary of clinics that promise guaranteed cures or that seem overly eager to proceed without a thorough assessment. Many individuals have found success by researching clinics that have been operating for a significant period and have a demonstrable track record of positive outcomes and a commitment to harm reduction principles. Exploring guides on navigating ibogaine treatment can offer valuable insights.
Furthermore, understanding the clinic’s approach to integration therapy is crucial, as this phase is vital for processing the insights gained during the ibogaine experience and translating them into lasting changes. A strong integration program typically involves individual therapy sessions, group support, and guidance on lifestyle adjustments. Reputable clinics will emphasize this as an integral part of the healing journey, not merely an optional add-on. The goal is to ensure that the profound insights from ibogaine are sustained and lead to long-term recovery and well-being.
Key Criteria for Selecting an Ibogaine Treatment Center
When selecting an ibogaine treatment center, several critical criteria must be evaluated to ensure safety, efficacy, and a supportive healing environment. Foremost among these is the medical safety infrastructure. A top-tier facility will have on-site medical professionals, including doctors and nurses, equipped to monitor vital signs continuously during the ibogaine experience and manage any potential medical emergencies, particularly cardiac events. This includes having access to necessary medical equipment like ECG machines and resuscitation equipment. Secondly, the qualifications and experience of the therapeutic team are paramount. Therapists and facilitators should possess a deep understanding of addiction, psychedelic-assisted therapy, and trauma-informed care, with a proven track record in administering ibogaine safely.
Another crucial criterion is the comprehensiveness of the pre-treatment screening process. Reputable centers conduct thorough medical and psychological assessments to identify contraindications, such as cardiovascular issues or psychiatric conditions that could be exacerbated by ibogaine. This screening is not just a formality but a vital step in ensuring patient suitability and minimizing risks. Decision-making should also consider the treatment setting and environment. The facility should be serene, comfortable, and designed to promote introspection and healing, offering privacy and a sense of security. Pitfalls include centers that rush the screening process, lack adequate medical supervision, or offer services in environments that are not conducive to deep therapeutic work.
Finally, the integration support provided post-treatment is a non-negotiable element. A robust integration program helps individuals process the profound experiences and insights gained during ibogaine therapy, translating them into sustainable behavioral changes and long-term recovery. This typically includes individual therapy sessions, group support, and resources for continued healing. Actionable steps involve asking detailed questions about each of these criteria, requesting to speak with staff members, and reviewing the clinic’s safety protocols and success rates. For those navigating this complex decision, understanding options through resources like understanding ibogaine treatment options can provide clarity.
The Process of Ibogaine Treatment: A Step-by-Step Guide
Pre-Treatment Screening and Preparation: Essential Safeguards
Embarking on ibogaine treatment necessitates a rigorous pre-treatment phase to ensure safety and optimize outcomes. This crucial stage begins with comprehensive medical and psychological evaluations. Clinicians assess potential participants for underlying health conditions, particularly cardiovascular issues, which can be exacerbated by ibogaine. A thorough review of current and past medications is also paramount, as drug interactions can be dangerous. For individuals in Canada, seeking ibogaine treatment in Canada often involves detailed questionnaires and possibly laboratory tests to identify any contraindications. Patients are educated about the profound nature of the ibogaine experience, including potential challenges and the importance of an open mindset. Developing a strong therapeutic alliance with the treatment provider is also a key preparation step, fostering trust and facilitating open communication throughout the journey. This preparation minimizes risks and maximizes the potential for profound healing.
Nutritional optimization and the discontinuation of certain substances are also part of the preparation. Patients may be advised to adopt a healthier diet and avoid stimulants or depressants in the weeks leading up to treatment. Hydration is emphasized, and some practitioners recommend specific supplements to support the body’s detoxification processes and enhance the overall experience. The psychological preparation involves setting intentions and understanding that ibogaine often brings repressed memories or emotions to the surface. This is where the support of a therapist or counselor can be invaluable, helping individuals process past traumas and prepare for the introspective journey ahead. Creating a supportive home environment for post-treatment recovery is also discussed, ensuring a smooth transition back to daily life.
The Administration of Ibogaine: Dosage and Monitoring
Administering ibogaine is a highly controlled process, typically conducted in a specialized clinic or retreat setting under the supervision of trained medical professionals. The dosage of ibogaine is highly individualized and depends on several factors, including the patient’s weight, metabolism, the specific substance they are seeking to overcome (if addiction is the primary concern), and their overall health status. A common starting point for addiction treatment might range from 12 to 20 milligrams per kilogram of body weight, but this can be adjusted significantly. The substance is usually administered orally, either as a capsule or a liquid extract, and the effects begin to manifest within 1 to 3 hours, with the peak experience occurring several hours later.
Continuous monitoring is absolutely essential throughout the ibogaine experience, which can last anywhere from 6 to 24 hours. Vital signs, including heart rate, blood pressure, and oxygen saturation, are closely tracked. Electrocardiograms (ECGs) are frequently employed to monitor cardiac activity, as ibogaine can affect heart rhythm. Patients are typically kept in a comfortable, quiet environment, often in a specialized treatment room, where they can safely navigate the intense introspective journey. The presence of experienced medical staff and therapists ensures that any adverse reactions are promptly managed and that the patient feels supported throughout the process. This attentive care is a hallmark of responsible ibogaine treatment in Canada and other reputable locations.
Post-Treatment Integration and Ongoing Support Strategies
The period following ibogaine administration is as critical as the treatment itself, focusing on integrating the insights gained and supporting the individual’s continued healing and growth. This phase, often referred to as integration, involves a range of therapeutic interventions designed to help patients process the profound experiences and psychological shifts that can occur. This typically includes one-on-one therapy sessions, where individuals can explore the memories, emotions, and patterns that surfaced during the ibogaine experience. Group therapy can also be beneficial, providing a sense of community and shared understanding among those who have undergone similar transformative journeys. The goal is to translate the intense psychological release into lasting behavioral change and emotional well-being.
Ongoing support strategies are vital for long-term success. This might involve developing relapse prevention plans, establishing healthy coping mechanisms for stress, and rebuilding social support networks. Many individuals find benefit in continued psychotherapy, exploring underlying issues that may have contributed to their initial struggles. Nutritional support and physical activity are also encouraged to promote overall health and resilience. For those who experienced profound shifts in their perspective on life, the integration phase also involves reconnecting with their values, goals, and sense of purpose. Access to resources like support groups or sober living environments can provide a crucial safety net during this delicate period. Exploring options for iboga capsules as part of a holistic wellness plan might also be considered for ongoing support and maintenance.
Beyond Ibogaine: Exploring Other Psychedelic Avenues
The Growing Interest in Psilocybin and MDMA for Mental Health
Beyond the significant role of ibogaine in addiction and trauma recovery, the therapeutic landscape of psychedelics has expanded dramatically, with psilocybin and MDMA emerging as prominent contenders for treating various mental health conditions. Psilocybin, the psychoactive compound found in magic mushrooms, is undergoing extensive research for its potential to treat depression, anxiety, and end-of-life distress. Clinical trials have demonstrated significant and lasting improvements in patients who receive psilocybin-assisted therapy, often after just a few sessions. The mechanism is thought to involve increasing neuroplasticity and facilitating profound emotional breakthroughs by allowing individuals to access and process difficult experiences in a new light. The careful curation of the therapeutic setting and the guidance of trained facilitators are paramount in harnessing psilocybin’s benefits safely and effectively.
Similarly, MDMA-assisted therapy is showing remarkable promise in treating post-traumatic stress disorder (PTSD). In controlled studies, MDMA appears to reduce the fear and defensiveness associated with traumatic memories, allowing individuals to revisit and integrate these experiences without being overwhelmed. This can lead to a significant reduction in PTSD symptoms, including intrusive thoughts, nightmares, and hypervigilance. The FDA has granted MDMA-assisted therapy for PTSD a Breakthrough Therapy designation, signaling its potential to revolutionize PTSD treatment. As research continues and regulatory pathways evolve, both psilocybin and MDMA are poised to become integral components of the psychedelic healing toolkit, offering new hope for conditions that have historically been challenging to treat.
Ketamine Therapy: A Proven Adjunct for Depression and Pain
Ketamine therapy has rapidly moved from an anesthetic agent to a well-established treatment for various mental health and chronic pain conditions. Its efficacy in rapidly alleviating symptoms of treatment-resistant depression has made it a cornerstone of modern psychiatric care. Unlike traditional antidepressants that can take weeks to show effects, ketamine often provides significant mood improvement within hours or days of administration. This rapid antidepressant effect is thought to be mediated by its action on glutamate receptors, promoting the growth of new synaptic connections in the brain and restoring neural pathways affected by chronic stress and depression. The availability of ketamine infusion clinics has made this treatment more accessible, offering a vital lifeline to those suffering from severe and persistent depressive episodes.
Beyond its psychiatric applications, ketamine is also proving highly effective in managing chronic pain conditions. Patients suffering from conditions like fibromyalgia, complex regional pain syndrome (CRPS), and neuropathic pain have found substantial relief through ketamine infusions. The analgesic properties of ketamine work through different mechanisms than traditional pain medications, offering a novel approach for those who have not responded to other treatments. For individuals seeking to explore psychedelics for pain management, ketamine presents a more readily available and FDA-approved option. The treatment is administered under strict medical supervision, with dosages and protocols tailored to the individual’s specific condition and response, ensuring both safety and therapeutic effectiveness.
Other Novel Psychedelic Compounds and Their Applications
The exploration into the therapeutic potential of psychoactive substances extends beyond the well-known ibogaine, psilocybin, MDMA, and ketamine. Researchers are investigating a range of other novel compounds, each with unique properties and potential applications. For instance, substances like DMT (dimethyltryptamine), often experienced in short, intense bursts through ayahuasca or synthesized forms, are being studied for their ability to promote profound spiritual experiences and offer rapid insights into complex psychological issues. The rapid onset and duration of DMT make it a subject of interest for rapid interventions, though its intensity requires careful preparation and integration.
Other compounds, such as LSD (lysergic acid diethylamide), which has a longer duration of action than psilocybin, are also being re-examined in therapeutic contexts for conditions like anxiety and depression. Research into 5-MeO-DMT, another potent naturally occurring tryptamine, is also gaining traction for its potential in treating depression and fostering spiritual emergence. The development of less psychedelic but still mind-altering compounds, sometimes referred to as “psychoplastogens,” aims to harness the neurobiological benefits, such as promoting neurogenesis and synaptic plasticity, without the intense subjective experience, potentially broadening their therapeutic accessibility. The careful study of these diverse compounds, like those found in certain 2C-B pills Canada, is essential for understanding their specific roles in mental wellness and addiction recovery.
Risks and Considerations for Psychedelic Healing in 2026
Potential Side Effects and Contraindications of Ibogaine
While ibogaine offers significant therapeutic potential, it is crucial to acknowledge and understand its potential side effects and contraindications. The most serious concern is its impact on the cardiovascular system. Ibogaine can prolong the QT interval on an electrocardiogram, increasing the risk of potentially fatal arrhythmias, especially in individuals with pre-existing heart conditions. Therefore, a thorough cardiovascular assessment, including an ECG, is a non-negotiable prerequisite for anyone considering ibogaine treatment. Other common acute side effects can include nausea, vomiting, tremors, and ataxia (loss of coordination). Patients often experience vivid dreams and intense introspection, which, while therapeutically beneficial, can also be emotionally challenging.
Furthermore, ibogaine can interact with various medications, particularly those affecting serotonin levels or cardiac function. A comprehensive medical history and a detailed list of all current medications are essential to avoid dangerous interactions. Contraindications also extend to individuals with severe liver or kidney disease, psychosis, or certain neurological disorders. The potential for psychological distress during the experience, including anxiety or paranoia, necessitates a safe and supportive therapeutic environment. Long-term or repeated use without proper medical guidance can also pose risks, including potential neurotoxicity, although research in this area is ongoing. Understanding these risks is paramount for informed consent and ensuring the safest possible ibogaine treatment.
The Importance of Safe Sourcing and Quality Control
Ensuring the safety and efficacy of psychedelic therapies hinges significantly on the quality and origin of the substances used. In the evolving landscape of psychedelic wellness, particularly concerning compounds like ibogaine and its derivatives, safe sourcing and stringent quality control are paramount. Illegally or unreliably sourced substances may be impure, contaminated with dangerous adulterants, or mislabeled, posing significant health risks to unsuspecting users. This is especially true when considering preparations intended for therapeutic use, where precise dosing and purity are critical for both safety and effectiveness. For individuals in Canada looking to explore therapeutic options, verifying the source of any authentic iboga capsules or ibogaine products is a non-negotiable step.
Reputable treatment centers and licensed dispensaries adhere to rigorous quality control measures, which include laboratory testing to verify the identity, purity, and potency of the substances. This meticulous approach minimizes the risk of adverse reactions stemming from unknown contaminants or incorrect dosages. When sourcing products, consumers should look for transparency regarding origin, manufacturing processes, and third-party testing results. The burgeoning market for psychedelic products, while offering accessibility, also presents challenges in maintaining these standards. Therefore, a commitment to responsible use involves prioritizing providers who demonstrate a clear dedication to safety, purity, and ethical sourcing practices, ensuring that the pursuit of healing does not inadvertently lead to harm.
Psychological Preparedness and Setting the Stage for Healing
The transformative power of psychedelic substances is not solely dependent on the compound itself but is profoundly influenced by the individual’s psychological state and the environment in which the experience takes place. Psychological preparedness is a cornerstone of safe and effective psychedelic healing, ensuring that individuals are emotionally and mentally equipped to navigate the profound insights and potential challenges that may arise. This preparation typically involves sessions with a trained therapist or guide who can help the individual explore their intentions, address any fears or anxieties, and set realistic expectations for the experience. Understanding that difficult emotions or memories may surface and learning healthy coping strategies beforehand is crucial for processing these experiences constructively.
The concept of “set and setting”—the individual’s mindset and the physical/social environment—is universally acknowledged as critical in psychedelic therapy. A supportive, safe, and comfortable setting, free from external distractions and potential stressors, allows the individual to surrender more fully to the experience. This might involve a quiet, aesthetically pleasing space, soft lighting, and comforting music. The presence of a trusted and experienced sitter or therapist provides a sense of security and guidance, ensuring that the individual feels supported throughout their journey. For those considering ibogaine for addiction, careful attention to preparation ensures that the intense introspective process can lead to lasting change, rather than overwhelming the individual. This comprehensive approach to set and setting, alongside potential therapeutic aids like iboga capsules, maximizes the potential for positive and sustainable healing outcomes.
The Future of Psychedelic Wellness: Predictions for the Coming Years
Increased Clinical Research and Evidence Generation
The trajectory of psychedelic medicine in the coming years is undeniably linked to a significant expansion in clinical research and evidence generation. As more studies emerge demonstrating the efficacy and safety of compounds like ibogaine, psilocybin, and MDMA for conditions ranging from addiction to depression and PTSD, the scientific community’s confidence and investment will grow. This intensified research will move beyond initial feasibility studies to larger-scale, multi-site clinical trials designed to meet the rigorous standards required for regulatory approval. The focus will shift towards understanding the long-term effects, optimal dosing protocols, and personalized treatment approaches, including exploring synergies with other therapeutic modalities. The insights gained from this robust evidence base will be crucial in legitimizing psychedelic therapies and paving the way for their broader adoption.
Furthermore, advancements in neuroimaging and biomarker research will offer deeper insights into the precise mechanisms by which psychedelics exert their therapeutic effects. This scientific precision will not only refine treatment protocols but also help to identify specific patient populations who are most likely to benefit from particular psychedelic interventions. The ongoing work with compounds like ibogaine, particularly in the context of complex addiction and trauma, will continue to yield valuable data, potentially uncovering new therapeutic applications. As this evidence base solidifies, it will form the foundation for evidence-based practice and inform public perception, moving psychedelics from the fringes of alternative medicine into the mainstream of evidence-informed mental healthcare.
Integration into Mainstream Healthcare Systems
The burgeoning body of scientific evidence is steadily paving the way for the integration of psychedelic therapies into mainstream healthcare systems. As compounds like psilocybin and MDMA move closer to regulatory approval for specific indications, healthcare providers will increasingly need to understand and incorporate these treatments into their practices. This transition will involve developing comprehensive training programs for physicians, therapists, and support staff, ensuring they possess the necessary knowledge and skills to administer psychedelic-assisted therapies safely and ethically. The establishment of clear guidelines for patient selection, treatment protocols, and post-treatment integration will be paramount in this process. For instance, understanding how to best manage patients seeking ibogaine treatment in Canada will require specialized training and infrastructure.
The economic implications of this integration are also significant. As psychedelic therapies prove their effectiveness, insurance providers will face increasing pressure to cover these treatments, making them more accessible to a wider population. This will likely involve a shift in how mental health services are funded and delivered, moving towards a more holistic and evidence-based approach. Pilot programs and specialized clinics are already beginning to emerge, offering a glimpse into what a future where psychedelic-assisted therapy is a standard option for various mental health conditions might look like. The challenge will be to scale these initiatives responsibly, ensuring that access is equitable and that the therapeutic integrity of these powerful interventions is maintained throughout the integration process. Innovations in delivery, such as potential take-home options for certain compounds under strict supervision, may also emerge as systems adapt.
Ethical Considerations and Responsible Use Guidelines
As psychedelic therapies gain traction, navigating the complex landscape of ethical considerations and responsible use guidelines becomes increasingly critical. Central to this is ensuring equitable access to these potentially life-changing treatments, preventing them from becoming exclusive to those with financial means. This involves addressing issues of cost, insurance coverage, and the potential for exploitation in emerging markets. Furthermore, the historical context of psychedelics, including their association with counter-culture movements and past prohibition, necessitates careful dialogue to ensure their re-integration is approached with respect and historical awareness.
Developing robust guidelines for practitioners is also a key ethical imperative. This includes establishing clear standards for training, competency, and professional conduct, as well as protocols for informed consent that fully disclose potential risks and benefits. The therapeutic relationship, particularly in potent experiences involving compounds like ibogaine, demands a high degree of trust, competence, and ethical integrity from the facilitator. Responsible use also extends to the consumer, emphasizing the importance of thorough research, personal preparedness, and choosing reputable sources. As the market for psychedelic products expands, including options like psychedelics for mental health, clear guidance on sourcing, dosage, and integration will be vital for safeguarding individuals and fostering a mature, ethical approach to psychedelic wellness.
Empowering Your Healing Journey: Resources for Canadians
Where to Find Certified Ibogaine Facilitators and Clinics
Navigating the landscape of psychedelic-assisted therapy requires careful consideration, especially when seeking ibogaine treatment. In Canada, regulatory frameworks are evolving, making it crucial to identify qualified professionals and reputable facilities. When searching for certified facilitators and clinics, prioritize those with a demonstrable track record, adherence to safety protocols, and a commitment to patient well-being. Look for credentials that signify formal training in psychedelic-assisted therapy, addiction counseling, or related medical fields. Many experienced practitioners have backgrounds in psychology, social work, or medicine, bringing a wealth of knowledge to the therapeutic process. It’s also vital to inquire about the clinic’s screening process, which should thoroughly assess your medical history, mental health status, and suitability for ibogaine therapy. Thorough pre-treatment evaluation is non-negotiable to mitigate risks and ensure a safe experience. Don’t hesitate to ask detailed questions about the facilitator’s experience with specific conditions you are seeking to address, such as substance use disorders or treatment-resistant depression.
Consider providers who offer comprehensive aftercare support, including integration sessions and follow-up therapy. This holistic approach is key to sustaining the positive changes initiated during the ibogaine experience. Resources like the Canadian Psychedelic Association (hypothetical resource for this example) often maintain directories of vetted practitioners and clinics, though direct verification of credentials and experience is always recommended. When evaluating potential clinics, look for clear communication regarding costs, treatment duration, and expected outcomes. Transparency is a strong indicator of a professional and ethical service provider. Remember, finding the right facilitator and clinic is a critical step towards a successful and transformative healing journey. Your due diligence ensures you are embarking on this path with trusted guidance and support.
Accessing Support Groups and Integration Services
The journey of psychedelic healing, particularly with substances like ibogaine, extends far beyond the administration of the treatment itself. Post-treatment integration is a cornerstone of lasting change, and robust support systems are essential. Support groups offer invaluable peer connection, allowing individuals to share experiences, challenges, and insights with others who understand the unique aspects of psychedelic healing. These communities can foster a sense of belonging and reduce feelings of isolation. When seeking integration services, look for therapists or counselors specializing in psychedelic-assisted therapy. These professionals can help you process the profound insights and emotional shifts that often arise from ibogaine experiences. Integration is not merely about reminiscing; it’s about actively translating insights into tangible life changes.
Effective integration involves exploring themes that emerged during the ibogaine session, such as trauma, core beliefs, and patterns of behaviour. Therapists can provide tools and strategies to navigate these complex psychological landscapes. Some clinics offer dedicated integration programs, while others can refer you to independent practitioners. When researching integration services, consider their approach: do they emphasize mindfulness, cognitive-behavioural techniques, or somatic therapies? The best approach often combines various modalities tailored to your individual needs. For those interested in exploring alternative avenues for mental wellness, understanding the potential of substances like 2C-B or delving into the broader spectrum of psychedelics for mental health can also be part of a comprehensive healing strategy, though direct guidance on their therapeutic application requires professional consultation.
Consider the accessibility of these services. Are they offered in person, virtually, or through a hybrid model? The ideal scenario involves ongoing support that helps you build resilience and implement positive changes in your daily life. Many online platforms and local community centres are beginning to host psychedelic integration circles. Researching these options thoroughly can help you find a supportive environment where you feel safe to explore and grow. The right support network amplifies the therapeutic benefits of ibogaine and empowers you to create a sustainable path toward well-being.
Understanding Your Options for Psychedelic Products in Canada
For Canadians seeking to explore the therapeutic potential of psychedelic compounds, understanding the available products and their responsible use is paramount. While ibogaine itself is primarily administered in controlled therapeutic settings due to its potent nature and potential risks, other psychedelic compounds are being explored for their wellness applications. This exploration requires a commitment to safety, legality, and informed decision-making. Consumers may encounter various forms of these substances, from raw plant materials to synthesized compounds. For instance, iboga capsules are sometimes sought for their potential in promoting introspection and supporting well-being, though their use outside of therapeutic contexts demands extreme caution and thorough research into dosage and preparation. It’s crucial to distinguish between research chemicals and compounds with established therapeutic applications. Always prioritize quality and authenticity when sourcing any psychedelic product.
In Canada, the legal status of many psychedelic substances varies. While some are classified as controlled substances, others are becoming more accessible for therapeutic or research purposes under specific medical guidelines. For individuals interested in purchasing products for personal wellness, such as authentic iboga capsules, it is imperative to engage with vendors who demonstrate transparency regarding sourcing, purity, and testing. Beware of unregulated online markets, as they often lack quality control and pose significant health risks. Responsible use also extends to understanding dosage, potential contraindications, and the importance of having a sober sitter or experienced guide present, especially for potent substances like ibogaine. Exploring resources dedicated to psychedelics for pain management or general wellness like iboga beyond addiction can offer insights into potential benefits, but always consult with qualified professionals before initiating any self-treatment. Being informed about the legal landscape and potential risks associated with each substance is the first step toward a safer exploration.
The landscape of psychedelic products in Canada is dynamic, with ongoing research and policy discussions influencing accessibility and understanding. As such, staying informed through reputable sources is vital. This includes understanding the differences between various compounds like psilocybin, MDMA, and ibogaine, and their unique pharmacological profiles and therapeutic applications. For those considering ibogaine treatment, consulting with experts at reputable clinics is the most secure route, as offered through resources that guide towards professional ibogaine treatment in Canada. Ultimately, responsible engagement with psychedelic products hinges on education, caution, and a commitment to personal safety and well-being.
For those embarking on their healing journey, identifying certified professionals, engaging in supportive communities, and understanding product options are crucial steps. This proactive approach empowers individuals to navigate the evolving landscape of psychedelic-assisted therapies with confidence.
When exploring your wellness transformation, resources like Mind Healing Shop can provide access to information and products aimed at supporting your journey.