As scientific inquiry deepens, substances like ibogaine are being scrutinized not just for their well-documented impact on addiction, but also for their unique potential in alleviating persistent pain. The exploration moves beyond mere symptom suppression, delving into the possibility of addressing the root neurological underpinnings of chronic suffering.
Understanding the Unconventional: Psychedelics and Pain Management in 2026
The year 2026 marks a significant juncture in the acceptance and scientific investigation of psychedelic substances for therapeutic applications. While historically viewed with skepticism, a growing body of evidence is reshaping perspectives on how compounds like ibogaine can be integrated into comprehensive pain management strategies. This evolving landscape recognizes that chronic pain is often a complex interplay of physiological and psychological factors, and that interventions targeting the brain’s neurochemistry can offer profound relief. The focus is shifting from solely managing symptoms to facilitating a deeper recalibration of the nervous system’s response to pain signals.
Shifting Paradigms: Beyond Traditional Pain Relief
Traditional pain relief often relies on pharmacological interventions such as opioids or non-steroidal anti-inflammatory drugs (NSAIDs). While these can be effective for acute pain or specific inflammatory conditions, they frequently fall short for chronic, complex pain syndromes, often leading to side effects, dependency, and a diminished quality of life. The paradigm is shifting towards understanding pain as a multifaceted experience influenced by neurotransmitter imbalances, emotional states, and even past trauma. This broader perspective opens the door for substances that can modulate neural pathways in novel ways, offering a more holistic approach to healing.
The Evolving Landscape of Psychedelic Research
Research into the therapeutic potential of psychedelics has witnessed a resurgence, moving from anecdotal accounts to rigorous clinical trials. Institutions globally are investigating these compounds for conditions ranging from depression and PTSD to addiction and, increasingly, chronic pain. This renewed interest is fueled by advancements in neuroimaging techniques that allow researchers to observe the intricate ways these substances interact with the brain. The scientific community is now more open to exploring how compounds like ibogaine, with their unique chemical structures, can facilitate neuroplasticity and alter pain perception pathways. This burgeoning field offers hope for patients who have found little solace in conventional treatments, paving the way for potential new therapeutic modalities.
Ibogaine: A Deep Dive into its Neurochemical Profile for Pain
Ibogaine, a naturally occurring psychoactive alkaloid derived from the roots of the *Tabernanthe iboga* shrub, possesses a complex neurochemical profile that distinguishes it from many other compounds explored for pain management. Its distinct interaction with various receptor systems within the central nervous system underlies its reported efficacy in both addiction treatment and, increasingly, in addressing persistent pain conditions. Understanding this intricate biochemical interplay is crucial for appreciating its therapeutic potential and for guiding safe and effective usage.
The Role of Ibogaine’s Active Compound, Ibogaine
The primary active compound within the *Tabernanthe iboga* plant is ibogaine itself, though other alkaloids like tabernanthine, tabernanine, and ibogaline also contribute to its overall effects. Ibogaine’s profound impact stems from its ability to interact with a multitude of neurotransmitter systems and receptors, acting as a modulator rather than a simple agonist or antagonist. This broad action profile is believed to be responsible for its capacity to interrupt cycles of addiction and potentially to re-regulate neural pathways involved in pain processing. Its unique ability to promote neurogenesis and neuroplasticity further sets it apart.
Mechanisms of Action: How Ibogaine Interacts with Pain Pathways
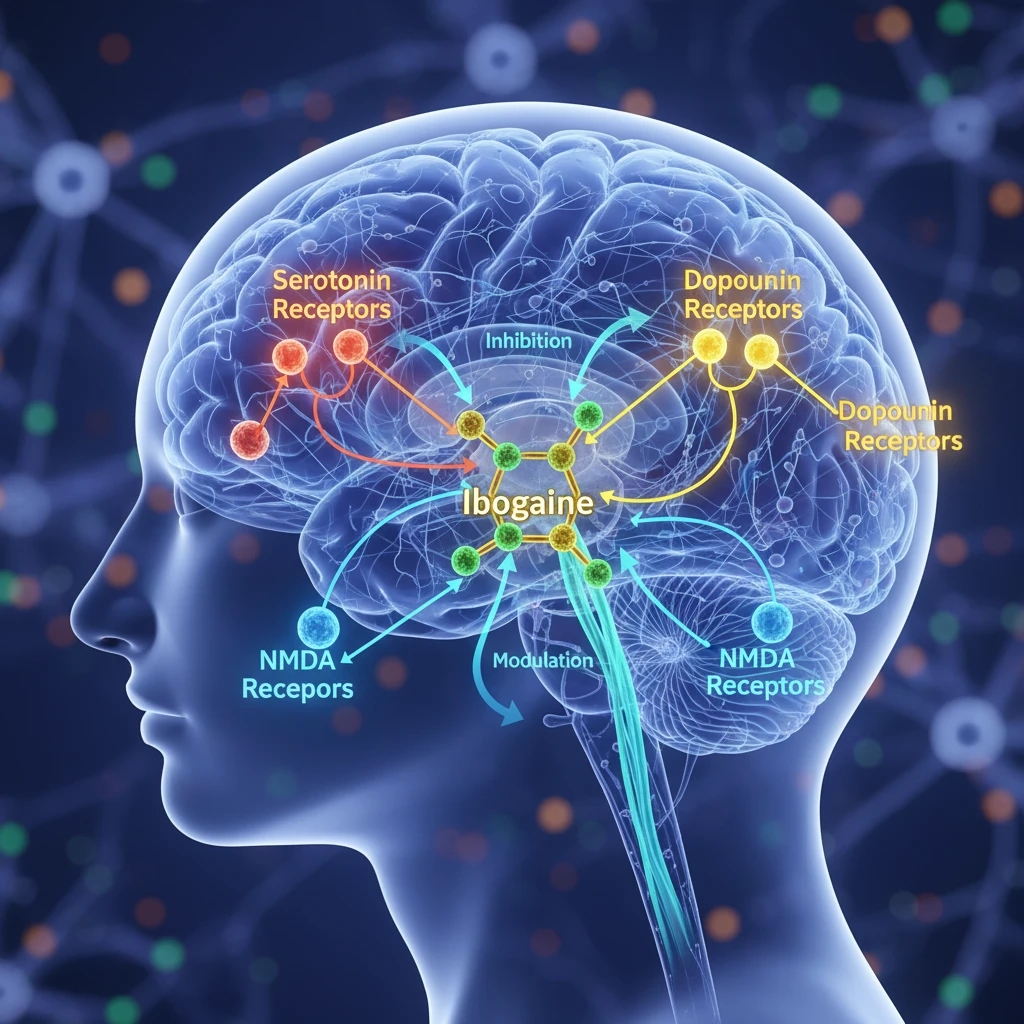
Ibogaine’s influence on pain perception is multifaceted, involving its interaction with several key neurological systems. It is known to interact with opioid receptors, potentially offering relief from pain by modulating the body’s natural pain-relieving pathways. Furthermore, its effects on serotonin and dopamine systems can influence mood and the emotional component of pain, which is often a significant factor in chronic suffering. The compound’s interaction with NMDA receptors is also a critical area of research, as these receptors play a role in synaptic plasticity and the phenomenon of central sensitization, a key factor in many chronic pain states.
Impact on Neurotransmitters: Serotonin, Dopamine, and NMDA Receptors
Ibogaine’s therapeutic effects are largely attributed to its complex interactions with critical neurotransmitter systems. It acts as an agonist at serotonin 5-HT2C receptors and a partial agonist at 5-HT2A receptors, influencing mood and perception. Its dopaminergic activity, including interaction with D2 receptors, can affect reward pathways and motivation, which are often disrupted in chronic pain conditions. Perhaps most significantly for pain modulation, ibogaine exhibits significant antagonism at NMDA receptors. This interaction is crucial because NMDA receptor overactivity is implicated in **excitotoxicity and the development of central sensitization**, a key mechanism in chronic neuropathic and inflammatory pain. By blocking NMDA receptors, ibogaine may help to **downregulate persistent pain signals** and promote neural recovery.
Ibogaine’s Potential in Chronic Pain Conditions
The unique pharmacological properties of ibogaine suggest significant potential for managing various forms of chronic pain that have proven resistant to conventional therapies. While research is ongoing, initial findings and anecdotal evidence point towards its capacity to address not only the physical sensations of pain but also the underlying neurological and psychological factors that perpetuate suffering. This includes conditions where inflammation, nerve damage, or central sensitization play prominent roles.
Evidence from Early Studies and Anecdotal Reports
While large-scale clinical trials are still emerging, existing evidence offers a compelling glimpse into ibogaine’s pain-relieving capabilities. Some early studies and numerous anecdotal reports from individuals who have undergone ibogaine experiences suggest a reduction in chronic pain, including conditions like fibromyalgia, chronic back pain, and complex regional pain syndrome. These accounts often describe not just a temporary analgesic effect but a more profound shift in pain perception, sometimes lasting for extended periods post-administration. The experiences highlight a potential for **long-term relief and a significant improvement in quality of life** for those suffering from persistent, debilitating pain.
Targeting Inflammation and Neuroinflammation
Chronic pain conditions are frequently associated with underlying inflammation, and in many cases, neuroinflammation – inflammation within the central nervous system. Research is exploring ibogaine’s potential to mitigate these inflammatory processes. Its interaction with cytokine pathways and its ability to modulate glial cell activity are areas of particular interest. By potentially reducing both peripheral and central inflammation, ibogaine could offer a novel therapeutic avenue for pain syndromes driven by these persistent inflammatory states. This is a crucial distinction, as many current treatments primarily focus on symptom management rather than addressing the root cause of such inflammatory pain.
Addressing Phantom Limb Pain and Neuropathic Pain
Phantom limb pain and other forms of neuropathic pain, stemming from nerve damage or dysfunction, represent some of the most challenging chronic pain conditions to treat. Ibogaine’s mechanism of action, particularly its interaction with NMDA receptors and its influence on neuroplasticity, positions it as a promising candidate for these conditions. By potentially **”resetting” aberrant neural signaling** and promoting the brain’s ability to adapt, ibogaine might help alleviate the intense, often burning or stabbing sensations characteristic of nerve-related pain. Further research in this area is critical for understanding its full therapeutic scope. For those seeking responsible exploration of such options in Canada, resources detailing usage guidelines are increasingly available.

Beyond Addiction: Ibogaine’s Broader Wellness Applications
While ibogaine’s transformative impact on addiction is well-documented, its therapeutic scope extends significantly into broader wellness applications, particularly concerning mental health co-occurring with chronic pain. Its ability to facilitate profound psychological shifts, coupled with its neurochemical effects, makes it a compelling subject for exploration in areas such as mood regulation, emotional processing, and recalibrating the brain’s fundamental pain perception. This holistic approach addresses not only the physical discomfort but also the psychological burden that often accompanies chronic suffering.
Potential for Mood Regulation and Depression Co-occurring with Pain
Chronic pain and mental health conditions like depression and anxiety are frequently intertwined, creating a debilitating cycle. Ibogaine’s interaction with serotonin and dopamine systems suggests a significant potential for mood regulation. By influencing neurotransmitter levels and promoting neurogenesis, it may help alleviate depressive symptoms and improve overall emotional well-being, which can, in turn, positively impact pain perception. Many individuals report a **lasting sense of emotional equilibrium and a reduction in the psychological distress** associated with their pain following ibogaine experiences. Exploring these facets aligns with a deeper look at ibogaine’s impact on overall wellness.
Enhancing Emotional Processing and Trauma Release
The subjective experience of ibogaine is often characterized by intense introspection and the revisiting of past memories and emotions. This process can be profoundly therapeutic for individuals who have experienced trauma, which is often a contributing factor to chronic pain. Ibogaine may help to **unlock and process suppressed emotions**, facilitating a release that can be cathartic and lead to a reduction in pain that is psychosomatically linked. This aspect of its action underscores its potential as a tool for comprehensive healing, addressing the mind-body connection integral to pain management.
The Concept of ‘Resetting’ the Brain’s Pain Perception
One of the most intriguing aspects of ibogaine’s potential in pain management is the concept of “resetting” the brain’s pain perception. Chronic pain can lead to maladaptive neural pathways where the brain becomes hypersensitive to pain signals, even in the absence of ongoing tissue damage. Ibogaine’s influence on neuroplasticity and its interaction with NMDA receptors may facilitate a neurobiological recalibration, effectively **”rebooting” the nervous system’s response to pain**. This profound shift can lead to sustained relief beyond the immediate pharmacological effects, offering a path towards a more balanced and less pain-centric existence. This aligns with the broader understanding of how psychedelics can contribute to healing and recovery.
Navigating the Practicalities: Sourcing and Legalities of Ibogaine in Canada
For Canadians exploring ibogaine’s potential for pain management, understanding the legal landscape and sourcing reliable products is paramount. As of 2026, Canada does not have explicit federal regulations permitting the sale or possession of ibogaine for recreational or wellness purposes outside of strict research contexts. This often leads individuals to seek alternative, albeit less regulated, avenues. It’s crucial to be aware that while some online vendors operate within Canada, the legal status remains ambiguous, and purchasing without proper authorization carries inherent risks. Research into the therapeutic applications of ibogaine is ongoing, but access for individual use is not widely sanctioned. Always prioritize obtaining information from reputable sources that discuss legalities transparently. Understanding these nuances is the first step towards a safe and informed exploration of ibogaine’s potential benefits for chronic pain conditions.
Understanding the Current Legal Framework (as of 2026)
In Canada, the legal status of ibogaine remains complex and largely restrictive. While the Controlled Drugs and Substances Act governs the possession, production, and distribution of many psychoactive substances, ibogaine itself is not explicitly listed in its schedules for general sale. However, its classification as a Schedule I drug under the UN Convention on Psychotropic Substances means that its import and export are tightly controlled. Authorized research and clinical trials, often conducted under specific exemptions, represent the primary legal avenues for ibogaine access. For individuals seeking ibogaine for personal use, particularly for chronic pain, navigating this landscape can be challenging. Some may explore options through medical exemptions, though these are rare and require rigorous justification. It’s essential to stay informed about evolving legislative discussions and any potential shifts in policy regarding therapeutic psychedelic substances. For a deeper dive into related compounds and their regulatory status, exploring resources on psychedelics for pain management in Canada can provide broader context.
The Importance of Reputable Sources for Ibogaine Products
Given the legal ambiguities and the potent nature of ibogaine, sourcing from reputable vendors is non-negotiable. The market can be inconsistent, with varying product quality and purity. Unverified sources may offer diluted or contaminated products, posing significant health risks. When seeking high-quality ibogaine products, look for vendors who are transparent about their sourcing, testing procedures, and product specifications. Websites that provide detailed information about the origin of their iboga root or synthesized ibogaine, along with third-party lab results verifying purity and potency, are generally more trustworthy. Customer reviews and testimonials, while not always definitive, can offer insights into a vendor’s reliability. For those in Canada looking for specific forms, resources like authentic iboga capsules in Canada can guide you toward established suppliers.
Considering Ibogaine Capsules vs. Ibogaine Powder
When considering ibogaine for pain management, the form in which it is obtained – capsules or powder – presents distinct practical considerations. Ibogaine powder offers flexibility in dosing, allowing for precise micro-dosing or custom preparation of larger doses under experienced guidance. However, it requires careful handling to avoid contamination and may be more challenging to dose accurately without specialized equipment. Ibogaine capsules, on the other hand, provide a more convenient and standardized approach to administration. They pre-measure the dose, simplifying usage and reducing the risk of accidental overdose or underdosing. This standardization can be particularly beneficial for individuals managing chronic pain who may need consistent and predictable therapeutic effects. For detailed guidance on using this form, exploring resources on ibogaine wellness can offer insights into effective integration strategies, regardless of the product form.
Responsible Use: Preparation and Integration for Optimal Outcomes
Engaging with ibogaine for pain relief is not a simple matter of ingestion; it demands thorough preparation and dedicated integration to ensure safety and maximize therapeutic benefits. The journey begins long before the substance is taken, involving comprehensive health assessments and mental readiness. This preparatory phase is critical for mitigating risks and setting the stage for a profound experience. Equally important is the post-experience period, where the insights and shifts gained during the ibogaine session are processed and woven into daily life. Without proper integration, the transformative potential can be fleeting. A holistic approach, encompassing physical, psychological, and environmental factors, is key to unlocking ibogaine’s capacity to address chronic pain and foster lasting well-being. Exploring various approaches to ibogaine wellness can illuminate the multifaceted nature of this practice.
Pre-Treatment Screening: Ensuring Safety and Suitability
Before considering ibogaine therapy for pain, rigorous pre-treatment screening is an indispensable step. This process aims to identify any contraindications that could pose serious health risks. A thorough medical history, including detailed information about cardiovascular health, is essential, as ibogaine can affect heart rhythm. Any pre-existing conditions, such as arrhythmias, hypertension, or liver disease, require careful evaluation by a qualified medical professional. Psychological screening is also vital; individuals with certain mental health disorders might be at a higher risk of adverse psychological reactions. This includes assessing for psychosis, severe anxiety disorders, or a history of severe psychiatric episodes. A comprehensive health assessment helps determine if ibogaine is a safe and appropriate option, and informs the dosage and therapeutic approach. If any concerns arise, consulting with specialists experienced in psychedelic-assisted therapies is highly recommended.
The Therapeutic Setting: Environment and Guidance
The environment in which ibogaine is administered significantly influences the therapeutic outcome. A safe, comfortable, and supportive setting is crucial for facilitating a positive and introspective experience. This typically involves a quiet space free from distractions, often adorned with calming aesthetics. Crucially, the presence of an experienced guide or facilitator is vital. These professionals provide crucial support throughout the session, offering reassurance, managing potential discomfort, and helping to navigate challenging emotional states. Their expertise ensures that the individual feels secure and understood, which is paramount for delving into deep psychological material often uncovered during ibogaine experiences. For those seeking structured support, exploring services that offer guidance in psychedelic therapy can be invaluable.
Post-Experience Integration: Maximizing Lasting Benefits
The period following an ibogaine experience is as critical as the experience itself for achieving sustained benefits, particularly in pain management. This phase, known as integration, involves processing the insights, emotions, and revelations that emerged during the session. It often includes several strategies: journaling about thoughts and feelings, engaging in mindfulness or meditation practices, and continuing dialogue with therapists or support groups. The goal is to translate the shifts in perspective and understanding gained under ibogaine’s influence into tangible changes in daily life, addressing the root causes of pain and developing healthier coping mechanisms. Consistent practice of these integration techniques helps solidify the therapeutic gains and prevent a relapse into old patterns. Understanding how to effectively integrate these experiences can be further enhanced by exploring resources on iboga’s role beyond addiction, as the principles of integration often share common ground.
Potential Side Effects and Risks Associated with Ibogaine Therapy
While ibogaine holds promise for pain management, it is a potent substance with a significant risk profile that necessitates careful consideration and medical oversight. Understanding these potential side effects is crucial for anyone contemplating its use. The physiological effects of ibogaine can be intense and multifaceted, affecting various bodily systems. Cardiovascular health is a primary concern, given ibogaine’s known impact on heart rhythm and function. Beyond cardiac risks, individuals may experience significant gastrointestinal distress, neurological effects, and a range of psychological responses that require careful monitoring. The complexity of these risks underscores the importance of professional medical supervision throughout the therapeutic process, ensuring that immediate interventions can be provided if adverse reactions occur.
Cardiovascular Considerations: A Critical Review
The most serious risks associated with ibogaine therapy are cardiovascular. Ibogaine is known to prolong the QT interval on an electrocardiogram (ECG), which can increase the risk of developing potentially life-threatening arrhythmias, such as Torsades de Pointes. This effect is dose-dependent and can be exacerbated by pre-existing heart conditions or the concurrent use of other medications that also affect cardiac conduction. Therefore, a thorough cardiovascular assessment, including an ECG, is absolutely essential prior to any ibogaine administration. Individuals with known heart disease, a history of arrhythmias, or significant electrolyte imbalances are generally considered poor candidates for ibogaine therapy. Close cardiac monitoring during and after the experience is imperative, and medical professionals must be prepared to manage any emergent cardiac complications. This careful attention to cardiac safety is paramount for mitigating severe adverse events.
Gastrointestinal and Neurological Side Effects
Beyond cardiovascular concerns, ibogaine can induce a range of gastrointestinal and neurological side effects. Commonly reported gastrointestinal issues include nausea, vomiting, and abdominal cramps, which can be severe and contribute to dehydration if not managed. These effects are often managed with antiemetic medications, administered under professional guidance. Neurologically, individuals may experience ataxia (loss of coordination), tremors, and temporary visual or auditory disturbances. Some users report transient periods of confusion, anxiety, or panic. While many of these effects are temporary and resolve as the substance clears the system, their intensity can be distressing and requires a supportive therapeutic environment. The potential for these side effects highlights the necessity of having trained personnel available to provide comfort and address any emergent symptoms promptly and effectively.
The Importance of Medical Supervision and Emergency Preparedness
Given the potent physiological effects and potential risks of ibogaine, medical supervision throughout the entire process is not merely advisable but absolutely critical. This supervision begins with comprehensive pre-treatment screening to identify contraindications and assess overall health status. During the ibogaine experience, trained medical professionals should be on hand to monitor vital signs, administer necessary medications to manage side effects like nausea or arrhythmias, and respond to any medical emergencies. Emergency preparedness extends to having a clear protocol in place for managing severe adverse reactions, including access to advanced cardiac life support if required. Furthermore, post-treatment monitoring is essential to ensure a stable recovery and to manage any lingering effects. The commitment to unwavering medical oversight is the cornerstone of minimizing harm and maximizing the safety of ibogaine-assisted therapy.
The Future of Ibogaine in Pain Management: Research and Development
The therapeutic landscape for pain management is continuously evolving, and ibogaine is emerging as a compound of significant interest in this field. While its historical use has primarily focused on addiction, its unique neurochemical properties suggest a broader potential for addressing chronic pain conditions. Ongoing research is exploring the mechanisms by which ibogaine might influence pain perception, reduce inflammation, and promote neuroplasticity—all crucial factors in managing persistent pain. The development of more targeted analogues or refined therapeutic protocols could further enhance its efficacy and safety profile. As scientific understanding deepens, the integration of ibogaine into multimodal pain management strategies may become more common, offering new hope for individuals struggling with debilitating pain.
Emerging Clinical Trials and Research Frontiers
The scientific community is increasingly exploring ibogaine’s potential beyond its well-known applications in addiction treatment. Current research frontiers are investigating its role in managing various chronic pain conditions, including neuropathic pain, inflammatory pain, and pain associated with conditions like fibromyalgia. Studies are examining ibogaine’s interaction with neurotransmitter systems, such as the opioid and NMDA receptors, which are central to pain signaling. Early-stage clinical trials are cautiously assessing safety and preliminary efficacy in controlled environments, often focusing on specific pain profiles. The development of ibogaine derivatives or related compounds that retain therapeutic benefits while minimizing adverse effects, particularly cardiovascular risks, is another key area of research. These efforts aim to refine dosing, administration methods, and patient selection criteria to optimize outcomes and broaden access within a regulated framework. The insights gained from these trials are crucial for understanding ibogaine’s pharmacological mechanisms in pain. For a broader view on related compounds, learning about technical overviews of ibogaine can provide deeper context.
The Role of Psychedelics in Personalized Pain Medicine
The advent of psychedelics, including ibogaine, is contributing to a paradigm shift towards personalized pain medicine. Traditional pain management often relies on a one-size-fits-all approach, which can be ineffective for many individuals and may lead to side effects like dependence. Psychedelics offer a novel pathway by potentially addressing the underlying neurological and psychological factors contributing to chronic pain, rather than just masking symptoms. Personalized approaches involve tailoring treatment plans based on an individual’s unique genetic makeup, medical history, psychological profile, and the specific nature of their pain. This could involve selecting the most appropriate psychedelic compound, determining optimal dosing strategies, and designing individualized integration protocols. By understanding the complex interplay of biological and psychological elements in pain, psychedelics can facilitate tailored therapeutic interventions that promote long-term relief and improved quality of life.
Challenges and Opportunities for Wider Acceptance
The path to wider acceptance and integration of ibogaine in mainstream pain management faces several significant challenges. The current legal status in many jurisdictions creates barriers to research and clinical application, demanding extensive regulatory hurdles. The potent psychoactive effects and associated safety concerns, particularly cardiovascular risks, necessitate stringent medical supervision and specialized training for practitioners, which are not yet widely available. Furthermore, public perception and ingrained stigma surrounding psychedelic substances can impede their acceptance by both patients and healthcare providers. Despite these challenges, opportunities for progress are emerging. Increased scientific research, growing evidence of therapeutic efficacy in clinical trials, and evolving public discourse around mental health and healing are paving the way for a more open dialogue. As more data becomes available and safety protocols are refined, the potential for ibogaine to become a recognized and valuable tool in the comprehensive management of chronic pain becomes increasingly feasible, especially within specialized therapeutic settings.
Comparing Ibogaine’s Pain-Relieving Mechanisms to Other Psychedelics
Ibogaine’s unique approach to pain management distinguishes it from many other well-known psychedelics. Unlike substances primarily acting on serotonin receptors, ibogaine interacts with a broader spectrum of neurotransmitter systems. Its complex pharmacology involves binding to NMDA receptors, dopamine transporters, and serotonin receptors, among others. This multi-target action is believed to contribute to its potent analgesic effects, which may extend beyond simple symptom masking. Research suggests ibogaine might influence central nervous system pathways involved in pain perception and processing, potentially offering a more comprehensive solution for chronic pain sufferers. This nuanced mechanism stands in contrast to substances like psilocybin, which are more predominantly serotonergic. While psilocybin can indirectly influence mood and perception of pain, ibogaine’s direct interaction with pain signaling pathways appears to be more pronounced. Understanding these distinct mechanisms is crucial for appreciating ibogaine’s potential role in pain relief, especially for conditions where conventional treatments have fallen short. For a deeper dive into the intricacies of ibogaine’s effects, exploring its technical overview can provide valuable insights into its biochemical interactions.
Ketamine, another substance increasingly explored for pain, shares some commonalities with ibogaine due to its NMDA receptor antagonism. However, ibogaine’s action at the sigma-1 receptor and its ability to modulate opioid receptors are areas where it diverges significantly. These interactions may play a role in its potential to reduce opioid withdrawal symptoms, a feature not typically associated with ketamine. Furthermore, the experience induced by ibogaine is often described as deeply introspective and transformative, potentially addressing the psychological components of chronic pain, which can be as debilitating as the physical sensations. This includes confronting underlying emotional traumas or beliefs that may exacerbate pain perception. While ketamine can offer rapid antidepressant effects and pain relief, ibogaine’s potential for neuroplasticity and its prolonged effects after a single dose suggest a different therapeutic paradigm. The exploration of these different pathways highlights the diverse ways psychedelics can engage with the human nervous system to alleviate suffering and promote healing.
Distinct Pathways: Ibogaine vs. Psilocybin vs. Ketamine
When examining pain relief, the neurobiological pathways targeted by ibogaine, psilocybin, and ketamine reveal significant differences. Psilocybin, often associated with profound shifts in consciousness, primarily acts on the 5-HT2A serotonin receptor. This activation leads to a cascade of effects that can alter mood, perception, and self-referential thought, indirectly impacting how pain is experienced. Individuals might report a greater sense of detachment from their pain or a shift in emotional reactivity to it. In contrast, ketamine is primarily known for its rapid NMDA receptor antagonist properties. This mechanism is highly effective for certain types of neuropathic and visceral pain, often providing significant relief in a clinical setting. Ibogaine, however, exhibits a more intricate pharmacological profile. It acts as an antagonist at NMDA receptors and also interacts with dopamine transporters and sigma-1 receptors, among others. This broad interaction spectrum is thought to contribute to its more comprehensive impact on pain signaling and its potential to address the neurobiological underpinnings of addiction and chronic pain simultaneously.
The subjective experiences and therapeutic outcomes associated with each substance further underscore these differences. Psilocybin-assisted therapy often focuses on processing emotional and psychological distress that may be linked to pain. The introspective journey can lead to new perspectives on life challenges, including chronic pain. Ketamine, typically administered in controlled medical settings, offers a rapid analgesic effect that can be crucial for acute or severe pain episodes. Ibogaine’s unique property lies in its potential for neuroplasticity and its reported ability to interrupt cycles of chronic pain and addiction. It may help reset the nervous system’s response to pain stimuli and address the underlying neurochemical imbalances that contribute to persistent discomfort. For those seeking to understand the foundational aspects of ibogaine’s action, a review of its deeper wellness aspects can be illuminating.
Synergistic Potential: Exploring Combined Therapies
The concept of combining ibogaine with other therapeutic modalities is an emerging area of interest, aiming to enhance pain relief and overall wellness outcomes. While ibogaine itself offers a powerful, multifaceted approach, integrating it with evidence-based practices could amplify its benefits. For instance, combining ibogaine therapy with structured physical rehabilitation programs may be particularly beneficial for individuals suffering from chronic pain conditions that affect mobility. The neuroplastic effects of ibogaine could potentially make the body more receptive to physical therapy, leading to improved function and reduced pain. Furthermore, incorporating psychotherapy alongside ibogaine treatment can address the psychological and emotional dimensions of chronic pain, such as depression, anxiety, and trauma, which often co-occur. This integrated approach recognizes that pain is a complex phenomenon with physical, emotional, and psychological components. The synergistic potential lies in addressing these interconnected factors simultaneously, leading to more sustainable relief and improved quality of life. Research into these combined therapies is ongoing, but initial insights suggest a promising future for holistic pain management strategies.
Exploring the synergistic effects of ibogaine with other plant-based medicines or well-established therapeutic techniques is also gaining traction. While caution is paramount, and such combinations must be undertaken with expert guidance, the potential for enhanced healing is significant. For example, some practitioners are investigating how ibogaine’s resetting properties might synergize with mindfulness-based stress reduction techniques to foster greater emotional regulation and pain acceptance. The goal is not merely to reduce pain intensity but to cultivate a more resilient and adaptive relationship with one’s body and mind. The exploration of iboga’s transformative power in psychedelic therapy opens doors to innovative combinations that could redefine the landscape of pain management. Ultimately, the pursuit of synergistic therapies aims to create comprehensive treatment plans tailored to the unique needs of each individual, moving beyond singular symptom management towards profound and lasting wellness.
Making an Informed Decision: When is Ibogaine a Viable Option?
Deciding whether ibogaine is a suitable option for pain management requires a thorough and individualized assessment. It is not a universally applicable solution and carries significant risks, necessitating a careful evaluation of personal health, motivations, and the nature of the pain. Key decision criteria include the type and chronicity of pain, previous treatment history, and the presence of any contraindicating medical or psychological conditions. For individuals with chronic, debilitating pain that has not responded to conventional therapies, ibogaine might be considered as a potential last resort. Its purported ability to interrupt neurochemical pathways associated with pain and addiction can offer a new avenue for relief. However, the decision should always be made in consultation with experienced medical professionals and facilitators who understand ibogaine’s complex pharmacology and potential side effects. Thorough patient education is paramount, ensuring the individual fully grasps the process, potential risks, and expected outcomes. Understanding essential usage guidelines for iboga capsules can be a starting point for this education.
The potential pitfalls of ibogaine treatment cannot be overstated. Serious cardiac risks, including QT interval prolongation and arrhythmias, are a primary concern, requiring comprehensive cardiac screening prior to administration. Neurological side effects, such as tremors and ataxia, can also occur. Furthermore, ibogaine can interact with various medications, potentially leading to dangerous complications. It is crucial to be transparent about all current prescriptions and supplements. The psychological effects can also be intense, and individuals with a history of psychosis or severe mental health conditions may not be suitable candidates. A comprehensive medical history and rigorous screening process are non-negotiable. For those considering ibogaine, resources like expert Canadian insights on safe iboga powder use can provide critical information regarding responsible preparation and administration protocols, highlighting the importance of professional oversight.
Assessing Individual Pain Profiles and Medical History
A fundamental step in determining the viability of ibogaine for pain relief lies in a meticulous assessment of an individual’s pain profile and medical history. This involves understanding the origin, intensity, duration, and specific characteristics of the pain. For example, neuropathic pain, inflammatory pain, and musculoskeletal pain may respond differently to ibogaine’s mechanisms. A detailed review of past medical records is essential, paying close attention to any history of cardiac abnormalities, liver or kidney dysfunction, neurological disorders, or psychiatric conditions. Pre-existing cardiac conditions are a significant contraindication due to ibogaine’s potential impact on heart rhythm. Comprehensive electrocardiogram (ECG) monitoring and cardiology consultations are often required. Equally important is a thorough understanding of current and past medication use, as drug interactions can be complex and dangerous.
Furthermore, the assessment must consider any co-occurring conditions, such as substance use disorders, which ibogaine is also investigated for. The interaction between pain and addiction is often bidirectional, and ibogaine’s unique properties may offer a pathway to address both simultaneously. However, this complexity necessitates expert guidance and careful consideration of the risks involved. For individuals in Canada seeking information on responsible use, exploring resources on deepening mental clarity through ibogaine wellness can provide a foundational understanding, but this must be complemented by a professional medical evaluation. Open and honest communication with healthcare providers about all aspects of one’s health is crucial for a safe and effective decision-making process.
The Role of Patient Education and Expectation Management
Effective patient education and rigorous expectation management are cornerstones of safely considering ibogaine for pain relief. Individuals must be thoroughly informed about the complex pharmacological profile of ibogaine, its known therapeutic effects, and its potential risks and side effects. This education should extend to the administration process, the typical duration of the acute effects, and the potential for residual psychological or physical experiences. Understanding that ibogaine is not a simple analgesic but a powerful psychoactive substance that can induce profound introspection and sometimes challenging emotional experiences is critical. Clear communication about the unpredictable nature of visionary states and the importance of integration afterward is vital. Resources such as those found in guides on responsible Canadian use of iboga capsules can offer a starting point for understanding practical application and safety considerations.
Managing expectations is equally important. While ibogaine shows promise for pain relief, it is not a guaranteed cure, and individual responses can vary significantly. Setting realistic goals and understanding that healing is often a process, not an instantaneous event, can prevent disappointment and undue stress. Patients need to understand that while ibogaine may provide a window of opportunity for healing, sustained benefits often require subsequent integration work, lifestyle adjustments, and potentially further therapeutic support. Avoiding the perception of ibogaine as a quick fix is crucial for fostering a sustainable approach to pain management. The focus should be on the potential for transformative healing and the creation of new coping mechanisms, rather than solely on the eradication of pain symptoms. Educating oneself and ensuring one is fully prepared for the intensity of the experience is a prerequisite for making an informed decision.
Considering Your Wellness Goals in the Context of Ibogaine Treatment
When contemplating ibogaine for pain relief, aligning its potential therapeutic effects with broader wellness goals is essential. Ibogaine’s capacity for profound introspection and its potential to address underlying psychological factors contributing to chronic pain mean that its use can extend beyond mere symptom management. For individuals seeking not just pain reduction but also a deeper understanding of themselves and a shift in their overall life perspective, ibogaine may offer a powerful catalyst. This could involve addressing patterns of avoidance, emotional distress, or existential concerns that have become intertwined with their pain experience. Prioritizing holistic healing over isolated symptom relief is key to maximizing the benefits of ibogaine. Exploring iboga’s journey beyond addiction towards wellness can illuminate how its applications can foster comprehensive personal growth.
It is also important to consider how ibogaine treatment fits into a long-term wellness strategy. The intense introspective experience can provide insights and motivation for significant life changes, such as adopting healthier habits, improving relationships, or pursuing meaningful activities. However, without adequate integration and support following the ibogaine experience, these potential benefits may not be sustained. Therefore, individuals should consider their readiness and capacity for post-treatment integration work. Evaluating one’s support system and commitment to ongoing self-care are crucial factors. For some, the ultimate wellness goal might be a return to a life unburdened by chronic pain, while for others, it may be the spiritual and personal growth that facilitates a more resilient and fulfilling existence, even in the presence of some physical discomfort. This self-reflection helps to ensure that ibogaine is chosen for reasons that align with a truly comprehensive vision of health and well-being.













Pingback: Rare Psychoactive Plants Canada Guide – Canada Botanals